Introduction
There are a number of drugs used in Stroke medicine and this is just a review. Aspirin and clopidogrel provide significant clinical benefit in patients with stroke and cardiovascular disease. However, it should be noted that aspirin or clopidogrel prevent only a small proportion of such events. Other agents e.g Prasugrel and Ticagrelor used in coronary disease are under evaluation for stroke.
Aspirin
Aspirin is a well-studied drug. Its pharmacological interest started with the fact that willow bark had anti fever properties. The Assyrians (4000 BC) and Sumerians (3500 BC), were aware of its medicinal merits. However, it took until the 1970s until we understood that aspirin acts to inhibit the enzymes COX 1 and COX 2 involved in prostaglandin synthesis. Sir John Vane, a British Pharmacologist proved the anticoagulant properties of aspirin by blocking the biosynthesis of prostaglandin, the pain messengers. He suggested that aspirin may reduce the risk of cardiovascular disease which led to use low-dose aspirin as a preventative measure in various cardiac conditions and then on to its application in stroke. It has several functions or characteristics and can act as an anti-inflammatory, Analgesic, Antipyretic, Antithrombotic and reduces TXA-B2. It is generally avoided in those under 16 as there is a risk of Reye's syndrome. Also avoid in Peptic ulcer disease, Allergy, Bleeding disorders, Asthma, G6PD. Side effects include GI irritation, GI ulceration, Reye syndrome, Anaphylaxis and allergy
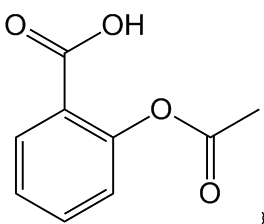
Aspirin (acetylsalicylic acid) acts by inhibiting platelet function by acetylating the platelet cyclooxygenase (COX) at the functionally important amino acid serine. This prevents arachidonic acid reaching the catalytic site of the enzyme and results in an irreversible inhibition of platelet-dependent thromboxane formation. Aspirin is predominantly a COX-1 inhibitor rather than COX-2 which is expressed by cytokines, inflammatory stimuli, and some growth factors. This explains low dose needed for antithrombotic (COX-1) activity and the higher doses needed for anti-inflammatory drug (COX-2). The optimum antiplatelet dose varies internationally - In the UK 75 mg/day and in the USA 81 mg/day and elsewhere 100 mg/day.
Trials
Dose [ Max dose 4 g/day]
- Ischaemic Stroke Protocol #1: Aspirin 300 mg PO for 2 weeks then Clopidogrel 75 mg od
- Ischaemic Stroke Protocol #1: Aspirin 300 mg and then 75 mg + Clopidogrel 75 mg od for 3 weeks then Clopidogrel alone
- Ischaemic heart disease: Aspirin 75 mg OD
- Anti-inflammatory 2-4 g/day in divided dose
- Analgesia 300-600 mg/day
Clopidogrel (Plavix)
Clopidogrel is a P2Y12 Platelet Inhibitor. The mechanism of action of clopidogrel is as a P2Y12 Receptor Antagonist. The physiologic effect of clopidogrel is by means of decreased platelet aggregation through its actions and belongs to the Thienopyridine-class of antiplatelets which irreversibly inhibit receptor called P2Y12 on platelets. It is a prodrug and needs liver metabolic pathways shared with other drugs such as PPIs. It is metabolised by CYP2C19. PPIs can reduce the formation of and so the effectiveness of Clopidogrel and should either be stopped if possible or switched to Pantoprazole or taken at different times at least 4 hrs apart.
Trials
- CAPRIE: C 75 mg + A 75 mg:
Combined Aspirin and Clopidogrel
Several trials have looked at combination therapy in different groups. The Chance trial was a randomised, double-blind, placebo-controlled trial conducted at 114 centres in China. 5170 patients within 24 hours after the onset of minor ischaemic stroke or high-risk TIA to combination therapy with clopidogrel and aspirin. (c or to placebo plus aspirin (75 mg per day for 90 days). All participants received open-label aspirin at a clinician-determined dose of 75 to 300 mg on day 1. The primary outcome was stroke (ischaemic or haemorrhagic) during 90 days of follow-up in an intention-to-treat analysis. Treatment differences were assessed with the use of a Cox proportional-hazards model, with study centre as a random effect.
Arms of trials
- Clopidogrel 300 mg loading + 75 mg/day for 90 days + Aspirin at a dose of 75 mg per day for the first 21 days then stopped
- Placebo + Aspirin 75 mg per day for 90 days
Results
- Stroke occurred in 8.2% of patients in the clopidogrel–aspirin group: Moderate or severe haemorrhage occurred in seven patients (0.3%) in the clopidogrel–aspirin group
- Stroke occurred in 11.7% of those in the aspirin group (hazard ratio, 0.68; 95% confidence interval, 0.57 to 0.81; P<0.001). Moderate or severe haemorrhage and in eight (0.3%) in the aspirin group (P=0.73);
- Both groups had a rate of haemorrhagic stroke was 0.3% in each group.
Dipyridamole
Dipyridamole (Persantin) was introduced in the late 1950s as an antianginal medication, as it was found to have coronary vasodilator properties and so increased coronary blood flow without significantly affecting myocardial oxygen consumption. Antiplatelet effects were subsequently demonstrated in animals and humans, and since then, the drug has been advocated as an antithrombotic agent.
Dipyridamole inhibits platelet phosphodiesterase, thereby preventing the degradation of cAMP (cyclic AMP) to AMP. An increased platelet cAMP reduces platelet reactivity by decreasing cytoplasmic calcium and inhibiting platelet prostaglandin synthesis. The adenosine transport blocking effects of dipyridamole also produce elevation of tissue adenosine levels. Furthermore, dipyridamole potentiates the effects of prostacyclin by increasing synthesis, enhancing release and inhibiting the metabolic degradation of prostacyclin.
Trials
- ESPS2 showed that combination A 25 mg BD + D 200 mg BD significantly reduced stroke risk
- ESPRIT: A 75 mg OD + D 200 mg BD reduced incidence 16 to 13 % with NNT of 100
Dipyridamole has no significant affect by itself and is usually used in collaboration with Aspirin 75 mg OD. Formulation Dipyridamole is usually given as Dipyridamole 200 mg Capsules bd with Apsiirn 75 mg OD. The main drawback of the drug is the headache which can be severe but usually settles after 1-2 days. The headache caused 9% of patients to quit Dipyridamole on ESPRIT. It can be almost thunderclap and is a testament to the vasodilator properties of the drug.
| Note: The plan is to keep the website free through donations and advertisers that do not present any conflicts of interest. I am keen to advertise courses and conferences. If you have found the site useful or have any constructive comments please write to me at drokane (at) gmail.com. I keep a list of patrons to whom I am indebted who have contributed. If you would like to advertise a course or conference then please contact me directly for costs and to discuss a sponsored link from this site. |