Learning objectives
|
Homocysteine
Numerous studies have demonstrated that plasma total homocysteine is a strong, graded, and independent risk factor for coronary heart disease and stroke. Elevated Total Homocysteine Levels in acute Ischaemic Stroke has been associated with long term mortality in some studies. There are several genetic disorders which predispose to vascular complications. Homocystinuria was first discovered in the early 1960s. It was found that some children born with the genetic disorder called homocystinuria, which causes the homocysteine levels to be very high, sometimes died at a very young age with advanced atherosclerosis.
Homocysteine is a naturally occurring sulfur-containing amino acid. It is a key intermediate of one-carbon metabolism and may serve as a surrogate marker of one-carbon metabolism status. It is involved in methionine synthesis and connects several B vitamins, including vitamins B-2, B-6, and B-12, folate. Compared with individual nutrients that partially mediate one-carbon metabolism, homocysteine may reflect the global network of one-carbon metabolism while simultaneously representing the optimum balance of these multiple nutrients. Homocysteine concentrations have been associated with several disease outcomes, including cancer, cardiovascular disease, neurodegenerative disease, and pregnancy complications.
Metabolism
One-carbon metabolism is a series of biochemical reactions that transfers methyl groups from one compound to another. This maintains DNA integrity by mediating the biosynthesis of purine and pyrimidine and the epigenetic signature by donating methyl groups for DNA methylation. Disruption of these metabolic pathways can lead to a deficiency of relevant nutrients and imbalance of relevant dietary factors has been associated with cancer and other health conditions. Hcy suppresses NO production by endothelial cells and platelets and increases generation of reactive oxygen species (ROS) by the release of arachidonic acid from the platelets. It also inhibits glutathione peroxidase and thus stimulates the proliferation of endothelial cells. Homocysteine is metabolised from methionine by three independent alternative pathways:
- Re-methylation
- Transmethylation to methionine
- Trans-sulfuration to cysteine
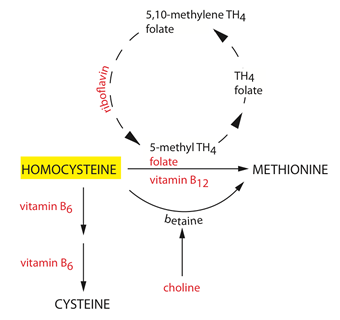
Most labs report normal ranges of homocysteine as about 4-15 micromoles/L but this can be > 100 micromoles/L in disease. It is felt that eating cereals that are fortified with folic acid, and to a lesser extent vitamins B6 and B12, can lower blood homocysteine levels but it has not been shown that there is a commensurate reduction in vascular risk. Homocysteine levels are not routinely measured in people with stroke or heart disease.
Hyperhomocystinaemia
- About: Gene mutation for methylene tetrahydrofolate reductase (MTHFR) C667Tx or methionine synthetase
- Aetiology: MTHFR is involved in the methylation of homocysteine to methionine
- Clinical: Arterial and venous thrombosis (intracranial) , Strokes, Acute coronary syndrome
- Investigations: high level of homocysteine in human blood
- Management: Folate supplementation + Pyridoxine + B12 , Low methionine and high cysteine diet , Trimethylglycine which promotes the conversion of homocysteine back to methionine
Homocystinuria
- About: Rare autosomal recessive disorder
- Aetiology: Cystathionine beta synthase deficiency
- Clinical: Marfanoid appearance , Learning disorder , Ectopic lentis and optic atrophy , Stroke due to arterial and venous thrombosis (intracranial)
- Investigations: Increased excretion of homocysteine in the urine , cystathionine beta synthase deficiency
- Management: Folate supplementation + Pyridoxine + B12 , Low methionine and high cysteine diet , Trimethylglycine which promotes the conversion of homocysteine back to methionine
References and further reading
| Note: The plan is to keep the website free through donations and advertisers that do not present any conflicts of interest. I am keen to advertise courses and conferences. If you have found the site useful or have any constructive comments please write to me at drokane (at) gmail.com. I keep a list of patrons to whom I am indebted who have contributed. If you would like to advertise a course or conference then please contact me directly for costs and to discuss a sponsored link from this site. |