Learning objectives
|
Herniation syndromes
The brain is contained within a bony box but there are also rigid structures within the skull which help to maintain the position of the brain and prevent excessive brain movements in response to rapid acceleration or deceleration forces. The falx lies in the midline and separates the lobes but also helps prevent excessive movement. The tentorium or "tent" separates the forebrain from the brainstem. Excessive forces within the skull can distort and squeeze neural structures which can be a sign of impending death. Seen in the context of rising ICP in the comatose patient. These are all neurosurgical emergencies and demand rapid escalation. There are three main forms
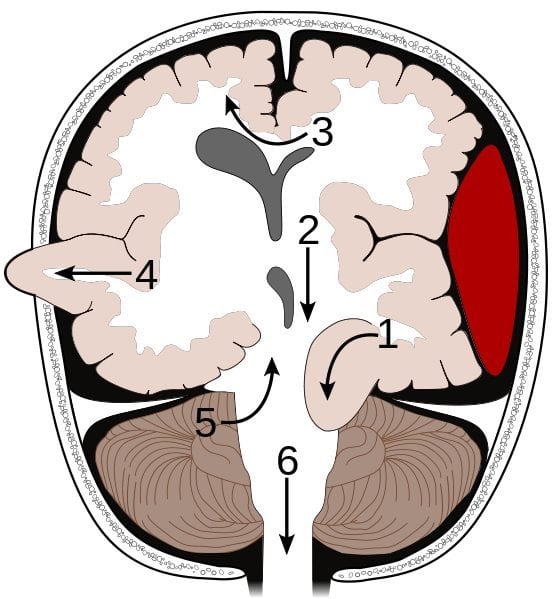
| No. | Syndrome | Segment affected | Details |
|---|---|---|---|
| [1] | Transtentorial | Medial temporal lobe (uncus), IIIrd nerve, PCA | Here an asymmetrical supratentorial mass or pressure gradient forces the uncus of the temporal lobe down beneath the tentorium 'tent' can result in an ipsilateral oculomotor paresis (dilated pupil, ptosis, down and out pupil) and compression of the posterior cerebral artery giving contralateral hemianopia. The shift forces the opposing cerebral peduncle against the edge of the tentorium causing contralateral hemiparesis to the peduncle. The indentation of the tentorium edge causes Kernohan's notch on the opposite cerebral peduncle. This is a false localising sign. Extensive brainstem ischemia may occur due to bleeding in the midbrain and upper pons with formation of Duret haemorrhages. |
| [2] | Central transtentorial hernation | Thalamus | There is a symmetrical downward movement of the thalamic region through the opening of the tentorium cerebelli with progressive coma |
| [3] | Subfalcine | Cingulate gyrus | Here the brain is pushed down and laterally under the falx separating right and left cortices. It is often due to a lobar mass or oedema or an extra-axial mass such as a subdural or extradural bleed. There may be compression of the anterior cerebral artery and stroke involving the as it is nipped by the edge of the falx with contralateral leg weakness. The lateral ventricles and brain midline will be distorted and shifted and can be seen on CT. Clinical effects in themselves mild but depend on the underlying cause |
| [4] | Transcavarial | Cortex | Seen after there has been a hemicraniectomy or there has been a fracture or some other skull lesion and the brain herniates outside the margins of the skull until the oedema settles. |
| [5] | Upward transtentorial herniation (“reverse coning”) | Cerebellum | So-called “reverse coning” can occur if an EVD is inserted for hydrocephalus due to a posterior fossa mass lesion. This leads to upwards transtentorial herniation of posterior fossa contents. |
| [6] | Transforaminal (Tonsillar "Coning") | Cerebellar tonsils and medulla | There is a huge ICP pressure that is forcing the brain down and out of the skull through the foramen magnum. Result is that the brainstem and cerebellar tonsils are forced down into the foramen magnum and pressure on the medulla leads to apnoea and death. |
Uncal herniation due to a SDH with Duret haemorrhages
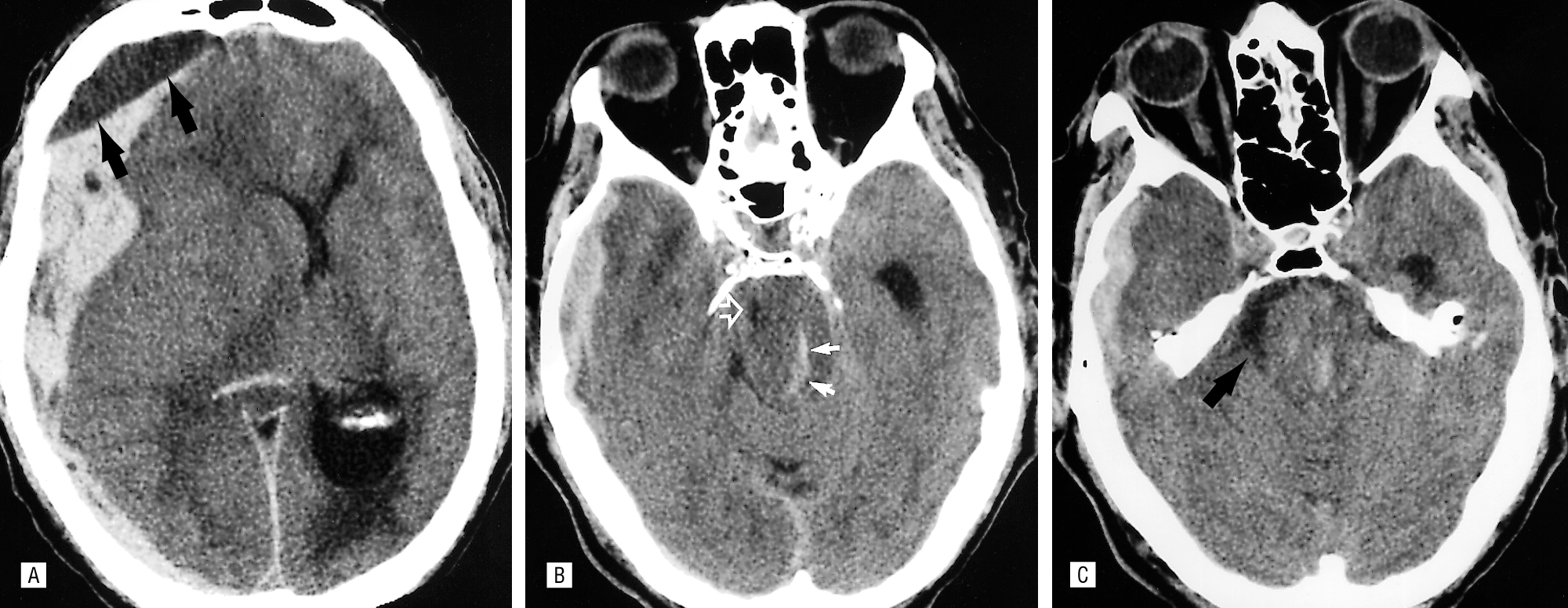
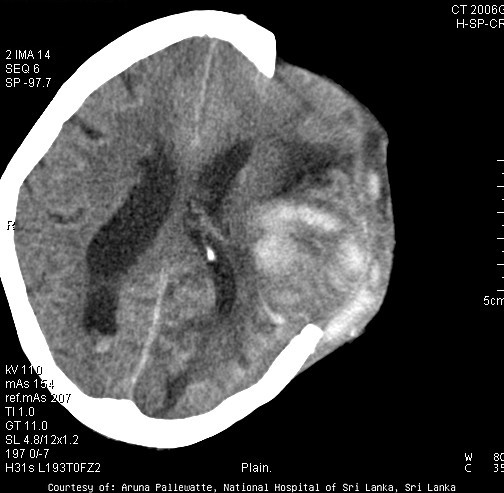
Trancavarial herniation
Clinical signs of Raised ICP
- Dilation of the pupil
- Confusion and/or Headache
- Depressed state or total loss of consciousness
- Droopy eye (Ptosis) due to a partial or complete third nerve palsy
- One sided weakness of the body (hemiparesis)
- Decreased heart rate (bradycardia)
- Obtunded and Deepening coma
- Irregular breathing, Respiratory depression or cardiac arrest (no pulse) that leads to death
Investigations
- Urgent CT and/or MRI
Management
- In advanced uncal herniation recovery to functional independence with these findings is a remote possibility. Increasing age, a greater than 6-hour interval between fixed pupils and craniotomy, and compression of basal cisterns all predict death. Palliation may be the plan. For those with less severe forms management may be urgent craniectomy and decompression or other neurosurgical management when there is a neurosurgical cause.
- Other options include using diuretics such as mannitol to reduce intracranial pressure and treatment of any acute hydrocephalus with an EVD
Next: >> Stroke Neuropathology |
| Note: The plan is to keep the website free through donations and advertisers that do not present any conflicts of interest. I am keen to advertise courses and conferences. If you have found the site useful or have any constructive comments please write to me at drokane (at) gmail.com. I keep a list of patrons to whom I am indebted who have contributed. If you would like to advertise a course or conference then please contact me directly for costs and to discuss a sponsored link from this site. |