Learning objectives
|
About
- A disorder of learned, voluntary actions resulting from neurological impairment
- An often unsuspecting cause of post stroke functional impairment which can be missed unless looked for.
- Seen in 1/3 of those in rehabilitation centres and nursing homes following left hemisphere stroke
Introduction
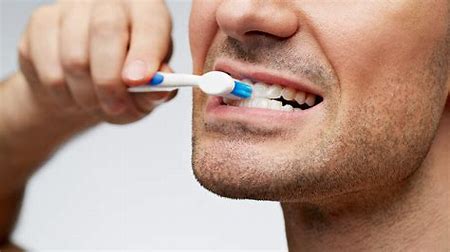
People with motor apraxia after a left hemispheric (dominant) stroke often have difficulty carrying out everyday activities such as making a hot drink. Some people cannot select the right object at the right time or have difficulty using objects (such as a spoon) correctly. Other difficulties include using toothbrushes, razors, combs, and brushes or in the kitchen an inability to use forks, knives, spoons, and other household equipment. There is insufficient evidence to support or refute the effectiveness of specific therapeutic interventions for motor apraxia after stroke.However it needs identified and actions undertaken to support improvement and help improve functional outcome and independence.
 |  |
Definitions
- Apraxia is defined as an inability to correctly carry out purposeful and often learned skilled movements and actions when this deficit is not caused by elemental motor or sensory deficits, abnormal involuntary movements, or cognitive disorders. A simpler definition is that is a higher order disorder of movement that is not due to elementary sensory and/or motor de’¼ücits.
- An impairment of the storage and transformation of motor representations in the brain, either through degradation of the semantic knowledge of gestures and tool use or through inability to translate the neural representations of higher level goals accurately into lower level patterns of muscle activation and inhibition.
- Liepmann proposed that left hemispheric lesions tend to cause bilateral upper limb apraxia and suggested a model of motor control in which the left parietal lobe stores a ŌĆśspaceŌĆōtime form pictureŌĆÖ of a movement. For a movement to be executed, its picture must be retrieved and activated and then be associated via cortical projections with the relevant motor engrams in the prefrontal regions. From here the information passes to the primary motor cortex before being fed down the corticospinal tracts. For the right upper limb to move the information remains contained within the left hemisphere, but for the left upper limb to move the information from the left parietal lobe must first be sent to the right prefrontal and frontal regions through the corpus callosum.
Anatomical basis
- Apraxia is a condition localised to the dominant left hemisphere
- Involves the supramarginal gyrus and deep white matter of the left parietal lobe.
- Apraxia can co-exist with a WernickeŌĆÖs aphasia, but they can also occur independently.
Types
- Ideational apraxia: A disorder in the performance of skilled activity because there is a disruption of the spaceŌĆōtime picture, in which the idea of the movement itself is lost or degraded. In concept of the action related to the object is impaired. A disturbance in the conceptual organisation of actions. The patient cannot pantomime tool use to command.
- Ideomotor apraxia: the idea of the movement is intact but there is an inability to map this accurately on to the motor engrams in the frontal lobes. A disorder in the initiation and execution of planned sequences of movement. The concept of the task is understood but the movements lack the correct force, direction and timing to achieve a motor goal. It is an impairment in timing, sequencing and spatial organisation of gestural movements. Tasks for example are - using a key, using a hammer, lighting a match. One key finding is the "body-part-as-object error", where the patient substitutes a body part for the tool in question e.g brushing the fingers through the hair when asked to demonstrate how it should be combed and to rub a finger against the teeth when asked to demonstrate how to use a toothbrush.
There are a whole variety of Apraxia
| Form | Definition |
|---|---|
| Ideational apraxia | Initially used to refer to impairment in the conceptual organization of actions, assessed with sequential use of multiple objects. Later de’¼üned as conceptual apraxia. |
| Conceptual apraxia | Impairment in the concept of a single action, characterized by content errors and the inability to use tools. |
| Ideomotor apraxia | Impairment in the performance of skilled movements, characterized by spatial or temporal errors in the execution of movements. |
| Limb-kinetic apraxia | Slowness and stiffness of movements with a loss of ’¼üne, precise and independent movement of the ’¼üngers. |
| Constructional apraxia | Dif’¼üculty in drawing or copying drawings of 3D structures. Impairment in the combinatory or organizing activity in which details and relationship among the component parts of the entity must be clearly perceived. |
| Developmental dyspraxia | Disorders affecting the initiation, organization and performance of actions in children. |
| Modality-speci’¼üc apraxias | Localized within one sensory system. |
| Pantomime agnosia | Normal performance in gesture production tests both on imitation and on verbal command, but poor performance in gesture discrimination and comprehension. Patients with pantomime agnosia can imitate pantomimes they cannot recognize. |
| Conduction apraxia | Superior performance on pantomime to verbal command than on pantomime imitation. |
| Visuo-imitative apraxia | Normal performance on verbal command with selectively impaired imitation of gestures. Also used to designate the defective imitation of meaningless gestures combined with preserved imitation of meaningful gestures. Optical (or visuomotor) apraxia Disruptions to actions calling upon underlying visual support. |
| Tactile apraxia | Disturbance of transitive hand movements for use of, recognition and interaction with an object, in the presence of preserved intransitive movements. |
| Upper/lower face apraxia | Impairment in performing actions with parts of the face. |
| Oral apraxia | Inability to perform skilled movements with the lips, cheeks and tongue. |
| Orofacial (or buccofacial) apraxia | Dif’¼üculties with performing intentional movements with facial structures including the cheeks, lips, tongue and eyebrows. |
| Lid apraxia | Dif’¼üculty with opening the eyelids. |
| Ocular apraxia | Impairment in performing saccadic eye movements on command. |
| Limb apraxia | Used to refer to ideomotor apraxia of the limbs frequently including the hands and ’¼üngers. |
| Trunk (or axial) apraxia | Dif’¼üculty with generating body postures. |
| Leg apraxia | Dif’¼üculty with performing intentional movements with the lower limbs. Task-speci’¼üc apraxias Gait apraxia Impaired ability to execute the highly practised, co-ordinated movements of the lower legs required for walking. Gaze apraxia Dif’¼üculty in directing gaze. |
| Apraxia of speech (or verbal apraxia) | Disturbances of word articulation. |
| Apraxia agraphia | A condition in which motor writing is impaired but limb praxis and non-motor writing (typing, anagram letters) are preserved. |
| Dressing apraxia | Inability to perform the relatively complex task of dressing. |
| Dyssynchronous apraxia | Failure to combine simultaneous preprogramed movements. |
| Orienting apraxia | Dif’¼üculty in orienting oneŌĆÖs body with reference to other objects. |
| Mirror apraxia | A de’¼ücit in reaching to objects presented in a mirror. |
| Lesion-speci’¼üc apraxias | |
| Callosal apraxia | Apraxia caused by damage to the anterior corpus callosum that usually affects the left limb. |
| Sympathetic apraxia | Apraxia of the left limb due to damage to the anterior left hemisphere (the right hand being partially or fully paralyzed). |
| Crossed apraxia | The unexpected pattern of apraxia of the right limb following damage to the right hemisphere |
Clinical: Screening tasks
- Pantomiming: Show me how you wouldŌĆ”Brush your teeth, Comb your hair, Hammer a nail,Use a pair of scissors
- Meaningful hand gestures: Salute, Hitch a lift, Wave goodbye
- Buccofacial apraxia: Lick your lips, Blow out a match, Drink through a straw
- Other Tasks which can be used in a functional setting
- Making a cold drink
- Putting paper in an envelope
- Hole punching paper and putting it in an A4 file.
Ideomotor Apraxia Performance errors
- Spatial orientation errors
- Temporal imprecision errors (timing errors)
- Errors of the force of movement
- Poor distal differentiation
- Body part as object ’ü« Gestural enhancement ’ü« Vocalisation
Ideational Apraxia Performance errors
- Using the wrong object
- Disordered Sequencing with omission or incomplete actions
- Blending sequences together
- Action overshoots what's required
- Action remains incomplete
- Perseveration
Management
- Therapy involvement to identify and focus on therapeutic strategy
- Involvement with Initiation, Execution, Control with Intervention, Instruction, assistance and feedback
References
- Cassidy A. The clinical assessment of apraxia. Practical Neurology 2016;16:317-322.
- Apraxia: a review. Progress in Brain Research, Vol. 164 ISSN 0079-6123
- Apraxia following stroke: Identification and interventions. Th├®r├©se Lebedis (Jackson)
- Cochrane. Interventions for motor apraxia following stroke. 23 January 2008
| Note: The plan is to keep the website free through donations and advertisers that do not present any conflicts of interest. I am keen to advertise courses and conferences. If you have found the site useful or have any constructive comments please write to me at drokane (at) gmail.com. I keep a list of patrons to whom I am indebted who have contributed. If you would like to advertise a course or conference then please contact me directly for costs and to discuss a sponsored link from this site. |